The University of Chicago cohort found arterial-ET difference, age, ventilator mode, vasopressor requirement, and APACHE II to be associated with mortality in a univariate analysis. In a separate analysis, the modified Enghoff equation ((P aCO 2–P ETCO 2)/P aCO 2) was used in place of the arterial-ET difference and did not alter the results. By multivariable analysis, only the arterial-ET difference remained significant ( P = 0.047). The ARDS Network derivation cohort demonstrated arterial-ET difference, vasopressor requirement, age, and APACHE III to be associated with mortality by univariable analysis. We then performed a separate retrospective analysis of patients with ARDS using University of Chicago patients ( N = 302) as a validation cohort. We first used publicly available databases from the ALTA, EDEN, and OMEGA ARDS Network trials ( N = 124) as a derivation cohort to test our hypothesis. We performed two separate exploratory analyses. 
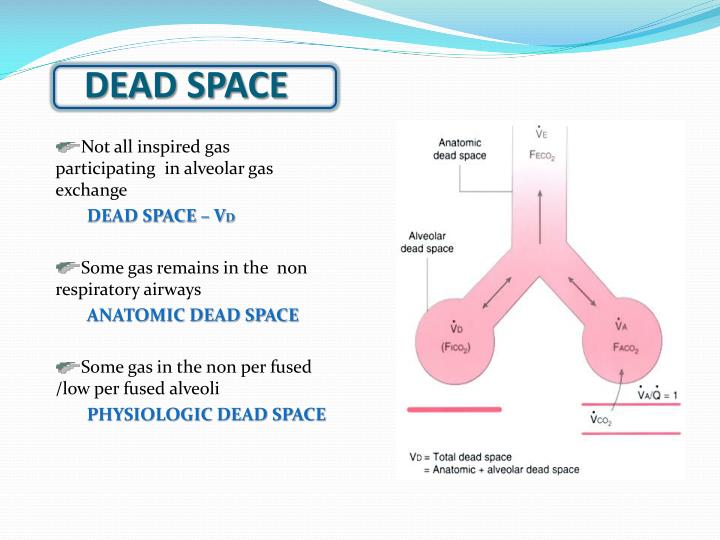
We hypothesized that early measurement of the difference between arterial and end-tidal CO 2 (arterial-ET difference), a surrogate for dead space fraction, would predict mortality in mechanically ventilated patients with ARDS. In acute respiratory distress syndrome (ARDS), dead space fraction has been independently associated with mortality. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
